
From here you can access a wide-range of information on child and maternity healthcare services, including guidance and support available, both in our hospitals and in the community.

From here you can access a wide-range of information on child and maternity healthcare services, including guidance and support available, both in our hospitals and in the community.
The Frontline Equality Assessment Tool (FEAT) has been designed to ensure that every service gets it right every time for all our patients.
Developed in response to feedback from our staff on areas where they feel NHSGGC could be doing better, the Tool also takes into account evidence from the experiences of our patients.
The FEAT focusses on assessing how we can fully meet the needs of all our patients within frontline services. It will be used by lead members of local service teams in collaboration with the Equality and Human Rights Team to look at patient flow and integration of inequalities sensitive practice.
This will involve reviewing how patient data is collected, how communication support is assessed, knowledge of protected characteristic-related issues and associated policies and protocols as well as the impact on discharge planning.
By translating the language of legislation into practical steps for staff, the FEAT offers a sense check which highlights both where there are gaps in services’ inequalities sensitive practice and where there are examples of good practice which could be replicated in other services.

“The Frontline Equality Assessment Tool is a great addition to our processes to enable us to understand and meet the needs of our patients with protected characteristics. Not only will it help us identify where we can take positive action but will also capture where good practice is underway and share across all wards and services.”

“Equality legislation can sometimes be seen as distinct or detached from the daily interactions that are at the heart of everything we do. We want to help change that perspective. The time we spend visiting departments will strengthen our understanding of equality legislation and its role in delivering effective, efficient and inclusive services.”
NHSGGC has a duty to remove access barriers for disabled patients. This takes the form of Disability Discrimination Audits (DDA) which involve conducting access audits in partnership with disabled people.
In addition to DDA audits, the Frontline Equality Assessment programme also includes a rapid assessment of a physical environment with proposed enhancements reported back to our Estates and Facilities Directorate.
We are currently carrying out a range of DDAs and FEAT reviews in Acute settings which aim to identify any adaptations required.

“We know that some aspects of the physical environment can still present barriers for some people who use our buildings. We are committed to a programme of ongoing improvement works as well as deigning space that will act as an enabler to staff, patients, carers and visitors.”
Healthy eating is essential to keep you and your baby healthy during pregnancy. Visit Ready Steady Baby |Eating well in pregnancy for more information about healthy eating during pregnancy.
During pregnancy, some vitamins are important to take. This page will tell you more about them and how to get these vitamins for free!
You will get Free Healthy Start vitamins throughout your pregnancy from your Midwife. These supplements contain folic acid, vitamin D and vitamin C to support you and your growing baby.

Healthy Start vitamins are suitable for vegetarians and free from wheat, fish, egg, and salt.
Contain no colours, flavours or preservatives.
Not suitable for vegans due to the source of vitamin D.
For those who are taking 5 milligram of Folic Acid, your GP will prescribe this. The Healthy Start Vitamins can be taken at the same time.
Ask your midwife for more information.
Healthy Start contains your recommended 400 micrograms of Folic Acid.
Folic Acid will help your baby’s spine properly during pregnancy.
Stops Neural tube defects such as Spina Bifida, which affects how the spine is formed.
During pregnancy, you need more folic acid to support your baby’s development, which is hard to get from your diet alone.
Healthy Start vitamins contains your recommended 10 micrograms of vitamin D.
Vitamin D helps our body absorb calcium to keep our bones and teeth healthy.
Low vitamin D levels can cause
• Seizures in babies after birth
• Vitamin D deficiency can cause problems and pain in the bones. This will be rickets in children.
Sources of vitamin D are limited. The best source of vitamin D is the sun and dietary sources are limited.
Healthy Start vitamins contain 70 micrograms of vitamin C.
• Vitamin C helps your body to absorb iron.
• Boosts your immune system.
• To help your body make collagen and protect your cells.https://www.nhsggc.scot/downloads/health-start/
Your Badgernet app will contain lots of information about pregnancy including Healthy Start.
Ready Steady Baby (NHS Inform)
Your Midwife will be there to support you throughout your pregnancy and will be happy to answer any questions.
This page provides information on person-centred visiting in our mental health wards. Information about visiting in all other areas can be found on our Person Centred Visiting page.
On admission to the ward, you will be asked about your preferences for visitors. Your family and/or significant others can also contribute to this. We will record this on a visiting form which will be kept with your care plan.
The importance of maintaining family connections with your children, when you are in hospital, is important. We will discuss this with you and your family at admission and during your hospital stay. Where possible, we will facilitate visits in a designated family area.
We have no set visiting times. This means you can be here to support your family member or friend at any time during the day. Please discuss with your family member or friend what they would like in terms of visits and what times would work best for you both, then talk to ward staff about your plans.
There may be times when visiting takes place in a communal area or visiting room, the nursing staff will advise where visiting is offered in each ward.
Should you need to access an area out with the dedicated visiting area, please speak to the nurse in charge.
In those Mental Health wards where visiting can only take place in dining rooms, family support during mealtimes will be discussed and agreed as part of individual visiting and care plans, in conjunction with the individual, the people who matter to them and staff.
To ensure a safe environment and that of yourself and others, please discuss with the nurse in charge what is safe and not safe to take into the ward. Examples of items not deemed safe are glass bottles, knifes, medications and plastic bags. Any electrical equipment should be handed into staff to be safety checked.
We recognise the benefits of having the opportunity to spend time with those visiting away from the immediate ward. However, there may be times when this is not possible. Please discuss this with the nurse in charge, and always let the nurse in charge know when you are going out of the ward with your family member.
It is important for staff to know when patients have returned to the ward. This ensures that staff maintain overall safety and activity on the ward, and allows staff to plan therapeutic engagement. In addition, this provides family members with the opportunity to feedback to staff on how the visit has gone and ask any questions regarding this.
It also equates to a day’s wages for more than 700 nurses, or more than 200 hospital consultants.
There are things we can all do to help reduce waste:
Contact your GP practice and ask to be referred to the GP practice pharmacy team to discuss if your prescription is still right for you.
It is important that patients check in regularly to make sure the prescription they receive is right for them.
If you receive a repeat or serial prescription, contact your GP practice and ask to be referred to the GP practice pharmacy team for a medicines review, or ask your community pharmacist for advice.
Our pharmacy teams are here to help your with your medicines, and they will work with you to make sure the medications you receive are right for you.
As well as being beneficial for your care, medication reviews help reduce medicines waste.
Medicines cannot be reused or recycled once they have been dispensed to you.
Over-ordering can lead to medicines going to waste if your prescription or health needs change. Please try to order only what you need, when you need it.
If anything has changed with your health, you may not need some of your medicines anymore. Please contact your GP practice or pharmacist to arrange a medication review.
Though you are not charged for your prescription medication, it still has a cost to the NHS, and the environment. It costs £11 on average for each individual medicine dispensed across Greater Glasgow and Clyde, and around 10% of the medicines dispensed, go to waste.

Primary Care is the front door to healthcare in NHSGGC, providing essential, first‑contact services to more than 1.3 million people across the region. For information, click here.
The GP Out Of Hours (GPOOH) service, part of Primary Care, in NHS Greater Glasgow and Clyde provides urgent care to patients when their regular GP service is closed. These services are designed to handle non-life-threatening medical issues that require attention outside regular working hours, such as evenings, weekends, and public holidays.
Primary Care is your first point of contact with healthcare and your front door to care with NHS Greater Glasgow and Clyde. Click here to view the new Primary Care hub.
The GP Out Of Hours service has been developed as an appointment-based model, that can be accessed by phoning NHS24 on 111.
This means we can help people get the right care in the right place.
Patients can access the GPOOH service in the evenings, overnight, across the whole weekend, and public holidays by contacting NHS 24 on 111.
If you require urgent non-life threatening care after your GP has closed you should phone NHS24 on 111.
Trained call handlers at NHS24 will assess your needs and if clinically appropriate will refer you to the GP Out of Hours service.
This new system also means that, where appropriate, patients can speak to a clinician over the phone or via a virtual consultation from the comfort of their own home, meaning they don’t have to travel to an urgent out of hours care centre.
The GP Out Of Hours service provides urgent primary care to patients outwith normal GP surgery hours. This includes evenings, weekends, and public holidays. This is accessed by calling NHS 24 on 111.
Patients can access the GPOOH service in the evenings, overnight and across the whole weekend and public holidays by contacting NHS 24 on 111.
Trained call handlers at NHS24 will assess the needs and if clinically appropriate will refer the patient to the GPOOH service.
This new system means that, where appropriate, patients can speak to a clinician over the phone or via a virtual consultation from the comfort of their own home, meaning they don’t have to travel to an urgent out of hours care centre.
With all patients being channelled through NHS 24 as a first point of contact, we can ensure that people are directed to the most appropriate type of care within the right environment, at the right time.
We have a fully integrated a telephone triage system into the patient care pathway, meaning where appropriate, patients can speak to a clinician over the phone or via a virtual consultation and may not even have to travel to an urgent out of hours care centre.
There are currently GP Out of Hours Centres at:
If you need a face-to-face appointment, you may be asked to attend a GP Out Of Hours centre outwith your local area. Those who need support travelling to a centre, patient transport can be arranged.
If you cannot travel, we also offer home visiting options.
If you cannot travel, we can also offer home visiting options and for those who need support to get to a centre and patient transport can be arranged.
With all patients being channelled through NHS 24 as a first point of contact, we can ensure that people are directed to the most appropriate type of care within the right environment, at the right time.
We have a fully integrated a telephone triage system into the patient care pathway, meaning where appropriate, patients can speak to a clinician over the phone or via a virtual consultation and may not even have to travel to an urgent out of hours care centre. Over half of our consultations are now carried out remotely within your own home. This ensures you can be seen by the right clinical person for your care. Being seen in the home setting also reduces waiting times, travel time and infection control risks.
Patient Transport is available to all patients. At time of arranging an appointment for a centre, the administrative staff will discuss travel arrangements to the centre for the patient. Any patients who indicate they don’t have transport means to travel to centre will be routinely offered patient transport. There is no charge for this service.
Carers can get the transport and child seats are also available and patient transport now includes accessibility for wheelchair users.
Yes it is available both to and from the centre.
UKHSA are currently managing an outbreak of meningococcal meningitis centred on Canterbury and Kent University. The outbreak has been confirmed to have been caused by a group B strain of the meningococcal bacteria, but it is currently unknown whether this is one of the group B strains included in available Men B vaccinations. At this stage, there is no evidence of wider community transmission beyond identified contact groups, and no cases linked to Scotland.
We are aware that as a result of the media attention on the outbreak, GP surgeries will be receiving queries from patients and parents, in particular with queries relating to meningitis vaccinations. We have updated this page to help address this.
Symptoms develop suddenly and can include:
These symptoms can appear in any order, and some may not appear.
The NHS inform pages include the vaccination schedules for children and young people. This includes the following meningitis vaccinations:
The MenB vaccination is offered to children under 2 who may have missed appointments in their first year, but is not available on the NHS for children over 2. Young people aged up to 25 are eligible to catch up on the MenACWY vaccination if they have missed this.
The Public Health Department do not hold vaccine records. The first step to checking your child’s vaccination history would be to look at their Red Book, but if you do not
have this, then you should ask your health visitor (for children under 5) or your child’s GP who can contact Child Health to request your child’s vaccination records.
The MenB vaccine is part of the routine NHS childhood immunisation programme and is offered to infants. Those under the age of 2 who have missed a Men B vaccine, are eligible for this in a catch-up form. For older children, teenagers, and adults, the MenB vaccine is not routinely offered on the NHS. There are a number of private providers available who will be able to administer Men B vaccine. You will understand that we cannot recommend any one private provider over another.
There are numerous strains of the meningococcal infection. The MenACWY vaccination gives good protection against MenA, MenC, MenW, and MenY. This vaccination is routinely offered in the UK to school pupils aged 13 or 14, but students and young adults who have not previously had the MenACWY vaccine may be eligible to receive it up to age 25. If anyone eligible has missed their Men ACWY vaccination, their GP can make a referral for this.
Additionally, for students attending universities in Glasgow, the NHS Greater Glasgow and Clyde Immunisations team run clinics on campus at the start of term offering vaccinations for eligible students who might have missed these.
Children aged 13 or 14 will be offered the MenACWY vaccination as part of the national routine schedule. Children who have missed this can catch up by being referred via their GP.
The development of effective vaccines has led to a huge decrease in childhood deaths. The World Health Organization (WHO) states: ‘The 2 public health interventions that have had the greatest impact on the world’s health are clean water and vaccines.’
As children develop they’re exposed to many risks, one of these risks being infections. Most of these will cause mild illnesses. However, despite great medical advances, infection can still cause severe illness, disability and, at times, death.
Before vaccines were available, many children in the UK died from diseases such as whooping cough, measles and polio. Despite successful immunisation programmes, the diseases that vaccines protect against do still exist.
The benefit of immunisation is that your child has the best possible protection against dangerous diseases. This can give you peace of mind.
What parents and caregivers need to know
Experts regularly review the vaccination programme to make sure it gives children the best protection. New research and changes in vaccine supply mean the vaccination schedule in Scotland has changed.
If your baby was born on or before the 30th of June 2024, they will already be mid-vaccine schedule and will remain on that schedule until it is complete. There is no action required from you and your baby will be invited for these vaccinations when the time approaches.
If your baby was born on or before the 30th of June 2024, they will continue to follow this schedule.
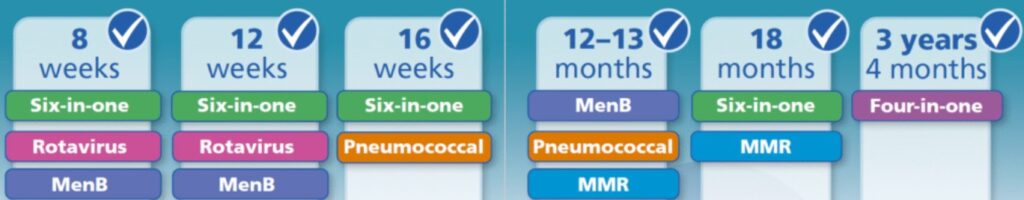
The following changes came into place on the 1st of July 2025.
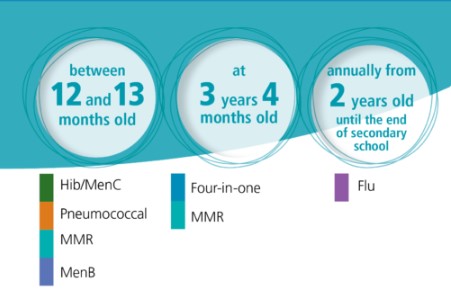
If your child turned one year of age on or after 1 July 2025 (DOB on or after 1 July 2024), they will pick up on this schedule from here:
What’s changing?
Some vaccines will now be given at different times, and a new appointment will be added when your child is 18 months old.
Who decides this?
The changes are based on advice from the Joint Committee on Vaccination and Immunisation (JCVI) – a group of independent experts who guide the UK and Scottish vaccination programmes.
What happens next?
There is no action required from you. You’ll be given clear information when it’s time for your child’s next vaccinations.
Why is this important?
Vaccines are the best way to protect your child from serious illnesses. These updates help make sure the programme stays safe, effective, and up to date.
MenB vaccination will now be offered from 12 weeks (previously 16 weeks).
Pneumococcal vaccination will now be offered from 16 weeks (previously 12 weeks).
The Hib/MenC vaccine (Menitorix) will no longer be available.
From January 2026, the MMRV vaccine will be offered as part of the routine childhood immunisation schedule. It replaces the MMR vaccine.
The MMRV vaccine protects against measles, mumps, rubella, and varicella (chickenpox). These are serious diseases that can be life-threatening.
Measles is a very infectious virus. It spreads easily though the air when people with the virus cough or sneeze. It can cause serious health complications, like pneumonia and encephalitis. In very serious cases, measles can be life-threatening.
Mumps is caused by a virus. It can cause permanent deafness, viral meningitis, and encephalitis. Mumps spreads through the air when people with the virus cough or sneeze, and is very infectious.
Rubella is caused by a virus. If caught in pregnancy, it can cause a miscarriage or affect the unborn baby. It can cause a condition called congenital rubella syndrome (CRS), which damages a baby’s sight, hearing, heart and brain. Rubella is spread through the air when people with the virus cough or sneeze, and is very infectious.
Varicella (chickenpox) is a highly infectious disease caused by a virus. Varicella is spread through direct contact with someone who is infected.
Read more about why your child should get the MMRV vaccine
The MMRV vaccine is offered to children as part of the routine childhood vaccination programme. When your child will be offered the vaccine depends on when they were born.
If your child was born on or after 1 January 2025
If your child was born on or after 1 January 2025, they’ll be offered 1 dose of the MMRV vaccine at both:
If your child was born between 1 July 2024 and 31 December 2024
If your child was born between 1 July 2024 and 31 December 2024, they’ll be offered a dose of the MMRV vaccine at:
If your child was born before 30 June 2024
If your child was born before 30 June 2024, they’ll be offered a dose of the MMRV vaccine at 3 years 4 months.
Introduction of a new 18-month appointment where the additional 6-in-1 (4th dose) vaccine will be offered.
The second dose of MMRV will be brought forward from the 3-year 4-month appointment to the new 18-month appointment.
Queries about scheduling
My children are different ages, will they be on different schedules?
Yes your children might be on different schedules as the schedule children follow is dependent on their date of birth. When changes to vaccination programmes happen, they must be rolled out on a phased basis to ensure NHS immunisation teams are able to deliver the vaccines effectively alongside other programmes. Changes to programmes are based on the advice of the Joint Committee on Vaccination and Immunisation (JCVI). These decisions are based on several factors, including the risk of the disease and the effectiveness of the vaccine.
If I delay my child’s vaccines, will they change schedules?
The schedule your child follows is dependent on their date of birth not when they attend for vaccination. Do not delay getting your child vaccinated – they will not change schedules. It’s important that vaccines are given on time to make sure your child has the best protection possible. Delaying or missing vaccine doses can put your child at risk of serious diseases and getting vaccines when they are due is the best way to protect your child.
The 6-in-1 vaccine, also commonly known as the DTaP/IPV/Hib/HepB vaccine, helps protect your child against:
Whooping cough is a disease that can cause long bouts of coughing and choking, making it hard to breathe. Whooping cough can last for up to 10 weeks.
Babies under one year old are most at risk from whooping cough. For these babies, the disease is very serious and can kill. It’s not usually as serious in older children. Before the pertussis vaccine was introduced, on average 120,000 cases of whooping cough were reported each year in the UK.
Diphtheria is a serious disease that usually begins with a sore throat and can quickly cause breathing problems.
It can damage the heart and nervous system and, in severe cases, can kill. Before the diphtheria vaccine was introduced in the UK, there were up to 70,000 cases of diphtheria a year, causing around 5,000 deaths.
Tetanus is a disease affecting the nervous system that can lead to muscle spasms, cause breathing problems and even kill. It’s caused when germs that are found in soil and manure get into the body through open cuts or burns.
Tetanus can’t be passed from person to person.
Polio is a virus that attacks the nervous system and can cause permanent paralysis of the muscles. If it affects the chest muscles or the brain, polio can kill.
Before the polio vaccine was introduced, there were as many as 8,000 cases in the UK during the polio epidemic. Because of the continued success of the polio vaccination, there have been no cases of paralytic polio in the UK for nearly 40 years (the last case was in 1984). Polio remains a threat with poliovirus traces found in London sewage in early 2022.
Being fully vaccinated is the best way to protect against becoming ill from polio. It’s important to make sure you and your child are up to date with your vaccines.
Hib is an infection caused by haemophilus influenzae type b bacteria. It can lead to a number of major illnesses such as blood poisoning (septicaemia), pneumonia and meningitis. The illnesses caused by Hib can kill if they’re not treated quickly. Before the Hib vaccine was introduced, there were about 800 cases of Hib in young children every year in the UK.
The Hib vaccine only protects your baby against the type of meningitis caused by the haemophilus influenzae type b bacteria – it doesn’t protect against any other type of meningitis.
More about haemophilus influenzae type b (Hib)
Hepatitis B (HepB) is a virus that infects the liver. Many people with HepB infection have no symptoms and don’t know they’re infected. Others have flu-like symptoms and yellowing of the skin (jaundice).
In children, HepB can persist for years and may eventually cause serious liver damage.
Babies can catch these serious diseases from birth, so it’s important to protect them as soon as possible.
All babies are eligible for the vaccine free on the NHS.
Your baby will be offered the 6-in-1 vaccine around 8, 12 and 16 weeks of age. Your local NHS immunisation team will contact you to let you know about their arrangements for your baby’s routine childhood immunisations.
Most NHS immunisation teams run special immunisation baby clinics. If you can’t get to the clinic, contact your local NHS immunisation team to make another appointment.
The meningitis B (MenB) vaccine helps protect against meningitis and septicaemia (blood poisoning) caused by meningococcal bacteria B.
Meningitis is inflammation of the lining of the brain and spinal cord. This causes pressure on the brain resulting in symptoms like:
Meningitis can progress very rapidly and can lead to:
It can even lead to death.
Septicaemia (blood poisoning) is a serious, life-threatening infection that gets worse very quickly. The risk of death is higher compared to meningitis.
The signs of cold hands and feet, pale skin, vomiting and being very sleepy or difficult to wake can come on quickly.
More about meningitis and septicaemia
Charlotte developed septicaemia (serious blood poisoning) through type B meningococcal disease (MenB) in 2010, before the MenB vaccine was introduced in the UK. Her mother Jenny talks about the impact on Charlotte and the rest of her family.
MenB is now the cause of most cases of meningococcal disease in Scotland. Although this infection isn’t common, MenB is extremely serious and can lead to permanent disability and death. The meningococcal bacteria can also cause local outbreaks in nurseries, schools and universities.
MenB infection is most common in babies and young children. This is because their immune systems aren’t yet fully developed to fight off infection. The highest number of cases are in babies around 5 months of age. This is why the first immunisations are offered to babies younger than this and have to be given at 2 and 4 months of age.
This vaccine helps protect babies against MenB, There are other vaccines, like MenC, that protect against some other types of meningococcal infections.
The MenB vaccine is routinely offered to all babies at 8, 16 weeks, and 12 to 13 months.
The MenB vaccine has been part of the routine childhood immunisation programme in Scotland since 1 September 2015. Your local NHS immunisation team will send you an appointment to bring your child in for their routine childhood immunisations.
Babies will be offered the MenB vaccine when they come in for their other routine immunisations at 8, 16 weeks and 12 to 13 months.
Find out how to contact your local NHS immunisation team regarding your vaccination appointment
If a baby is due their MenB vaccine, please ask your pharmacist about paracetamol for them. Fever can be expected after any vaccine but is more common when the MenB vaccine is given with the other routine immunisations at 8 and 16 weeks of age. This is why it’s recommended that babies gets infant paracetamol when getting these immunisations to prevent and treat fever.
The rotavirus vaccine helps protect babies against rotavirus.
Rotavirus is a virus that infects the gut (tummy), causing severe diarrhoea and vomiting. Most babies get sick (vomit) or have diarrhoea at some time and recover fully after a few days. However, sickness and diarrhoea caused by rotavirus can lead to dehydration (loss of body fluids). Dehydration can be very dangerous for babies and young children and can require hospital treatment.
Before the vaccine was introduced in 2013, around 1200 babies in Scotland had to go to hospital every year with rotavirus.
The rotavirus immunisation protects a baby against this illness.
The most important thing you can do is have the baby immunised against rotavirus, as part of the Routine Childhood Immunisation Programme in Scotland.
In countries where babies already get the rotavirus vaccine there’s been a big drop in the number of babies and young children going to hospital because of the virus.
With lots of younger babies having the immunisation the chances of it spreading are reduced. Rotavirus causes fewer problems in older children, and it’s rare in adults.
The rotavirus immunisation is offered to all babies in Scotland.
The rotavirus vaccine is normally given with the baby’s other routine immunisations at 8 weeks and again at 12 weeks of age. Your local NHS immunisation team will invite you for the vaccination, so there’s no need to book an appointment.
The pneumococcal vaccine helps protect against illnesses and conditions caused by pneumococcal bacteria.
Pneumococcal infection is caused by pneumococcal bacteria. It can cause serious illness such as pneumonia, and is one of the most common causes of meningitis (an infection of the lining of the brain).
Pneumococcal infection can cause:
Children under 2 years of age and children with certain health conditions have a higher chance of becoming unwell with pneumococcal infection.
Up to 60% of children carry pneumococcal bacteria in the back of their nose and throat. They constantly pass these bacteria around by coughing, sneezing and close contact.
The pneumococcal vaccine provides some protection against meningitis caused by pneumococcal infection, and against other conditions such as severe ear infections and pneumonia caused by pneumococcal bacteria.
This vaccine doesn’t protect against meningitis caused by other bacteria or viruses.
Some children are at an increased risk from pneumococcal infection. All at risk children will be offered the vaccine according to the routine childhood immunisation programme. If you aren’t sure about your child’s health or need further advice, speak to your health professional.
If a baby is eligible, they will be offered the pneumococcal vaccine when they’re 12 weeks old, with a booster dose given between 12 and 13 months. The pneumococcal booster dose between 12 and 13 months is usually given at the same time as the Hib/MenC, MMR and MenB vaccines.
In addition to this some children and adults aged from 2 to 64 years old, who are at a higher risk of developing a pneumococcal infection than the general population, will be offered additional pneumococcal vaccinations.
Your local NHS immunisation team will contact you to let you know about their arrangements for the baby’s routine childhood immunisations.
The Hib/MenC vaccine helps protect a child against 2 of the causes of meningitis and septicaemia (blood poisoning). This vaccine will help protect the child through early childhood.
Hib is an infection caused by Haemophilus influenzae type b bacteria. It can lead to a number of major illnesses such as septicaemia (blood poisoning), pneumonia and meningitis.
More about Haemophilus influenzae type b
Meningitis is inflammation of the lining of the brain and spinal cord. This causes pressure on the brain resulting in symptoms like:
Meningitis can progress very rapidly and can lead to:
It can even lead to death.
Septicaemia (blood poisoning) is a serious, life-threatening infection that gets worse very quickly. The risk of death is higher than with meningitis.
The signs of cold hands and feet, pale skin, vomiting and being very sleepy or difficult to wake can come on quickly.
A child will be offered a dose of the combined Hib/MenC vaccine between 12 and 13 months of age to:
The Hib/MenC vaccine doesn’t protect against meningitis and septicaemia (blood poisoning) caused by:
A baby will be offered the Hib/MenC vaccine at 12 to 13 months. Your local NHS immunisation team will contact you to let you know about their arrangements for the baby’s routine childhood immunisations.
Most NHS immunisation teams run special immunisation baby clinics. If you cannot attend your appointment contact your NHS immunisation team to make another.
Find out how to contact your NHS immunisation team regarding the baby’s vaccination appointment
The MMR vaccine is given in 2 doses and helps protect against measles, mumps and rubella. Find out more about the vaccine, and when and where to get it.
The MMR vaccine helps to protect people against measles, mumps and rubella. It’s sometimes also offered to adults who missed their childhood immunisations.
Measles, mumps and rubella are highly infectious diseases. They can cause serious medical complications.
A high number of people in Scotland have had the MMR vaccine. This means there’s been a big reduction in the number of people catching these diseases.
All babies and children in Scotland are eligible for the MMR vaccine.
They’ll be offered the MMR vaccine in 2 doses:
Although normally given at these times, if it’s missed, it can be given at any age.
Some young people and adults who missed out on their MMR vaccine may also be eligible, like those who are a planning a pregnancy. If you didn’t have 2 doses of the MMR vaccine as a child, you can contact your local NHS immunisation team to discuss your eligibility.
The 4-in-1 vaccine, also known as the DTaP/IPV or dTaP/IPV vaccine, helps protect your child against:
Whooping cough is a disease that can cause long bouts of coughing and choking, making it hard to breathe. Whooping cough can last for up to 10 weeks.
Babies under one year are most at risk from whooping cough. For these babies, the disease is very serious and can kill. It’s not usually as serious in older children.
Whooping cough germs can be spread from person to person through close contact.
Diphtheria’s a serious disease that usually begins with a sore throat and can quickly cause breathing problems. It can damage the heart and nervous system and, in severe cases, can kill.
Diphtheria germs are spread from person to person through close contact.
Tetanus is a disease affecting the nervous system that can lead to muscle spasms, cause breathing problems and even kill.
It’s caused when germs found in soil and manure get into the body through open cuts or burns. Tetanus can’t be passed from person to person.
Polio is a virus that attacks the nervous system and can cause permanent paralysis of the muscles. If it affects the chest muscles or brain, polio can kill.
The polio virus is usually spread from person to person, or by swallowing contaminated food or water.
Before the polio vaccine was introduced, there were as many as 8,000 cases in the UK during the polio epidemic. Because of the continued success of the polio vaccination, there have been no cases of paralytic polio in the UK for nearly 40 years (the last case was in 1984). Polio remains a threat with poliovirus traces found in London sewage in early 2022.
Being fully vaccinated is the best way to protect against becoming ill from polio. It’s important to make sure you and your child are up to date with your vaccines.
The vaccine boosts the immunisations that were given to your child at 8, 12 and 16 weeks of age – boosting protection against pertussis (whooping cough), diphtheria, tetanus, and polio.
This vaccine’s offered to children aged over 3 years 4 months at the same time as they are offered the MMR vaccine. It’s also used for a primary course of immunisation in children over 10 years old and adults.
Your child will be offered the 4-in-1 vaccine at around 3 years and 4 months. Your local NHS immunisation team will contact you to let you know about their arrangements for your child’s routine childhood immunisations.
Most NHS immunisation teams run special immunisation clinics. If you can’t get to the clinic, contact your local NHS immunisation team to make another appointment.
Immunisation (vaccination) information in other languages
Evidence shows the HPV vaccine helps protect people from HPV-related cancers. The human papillomavirus (HPV) vaccine is offered to every S1 pupil in Scotland.
Getting the vaccine now protects you against future risks. HPV can lead to cancers like:
The HPV vaccine also protects you against over 90% of genital wart infections.
Every person in Scotland aged 11-13 will be offered the HPV vaccine free of charge.
You should not have some vaccines if you’ve had a confirmed serious (anaphylactic) reaction to:
The GARDASIL 9 vaccine is used in Scotland.
Gardasil 9 helps protect against 9 types of HPV.
The vaccine protects against HPV types 16 and 18, which are the cause of most cervical cancers in the UK (more than 80%). The vaccine also protects against types 31, 33, 45, 52 and 58, which cause an additional 15% of cervical cancers.
The vaccine also protects against 2 other types of HPV. These cause around 90% of cases of genital warts.
The HPV vaccine is not a live vaccine. It cannot cause HPV.
The vaccine is the safest and most effective way to protect against HPV.
You’ll be offered the HPV vaccine as part of the school-based immunisation programme. Vaccines are given by your local NHS immunisation team.
Your school will tell you when vaccination sessions are taking place.
Find out more about the vaccinations you’ll be offered at school
If you have any questions on the day, you can speak to the person giving you the vaccine.
If you missed your vaccination and you’re still at school
If you miss your HPV vaccination, there will be further opportunities to get it. For example, you may be offered a rescheduled vaccination appointment next year.
If you’re unsure if you’ve missed any other vaccines, you should
first check your red book. If you do not have a red book, or it has gone missing, you can check with your local NHS immunisation team.
Young people not in mainstream education
You’re also eligible for the HPV vaccine if you’re:
Please contact your local NHS immunisation team to arrange your appointment.
If your child is home schooled and has missed out on any vaccinations and you with them to be vaccinated. Then please ask your GP Practice to refer you to the Child Vaccination Team for this. On receipt of the referral the team will be in touch with you to arrange this.
If you’ve missed your vaccination and have now left school
If you’ve left school and you didn’t get your HPV vaccine when you were eligible, you may still be able to get it up until you turn 25.
This only applies to:
Your local NHS immunisation team can confirm if you’re eligible. They can also explain how to get the HPV vaccine in your area.
If you / your child does not attend school or has missed vaccinations given in school, please contact the School Team listed under FAQs ‘School Team Contact Details’.
You should be given a consent form and leaflet by your school. You and your parent or carer should chat about the information. Both you and your parent or carer should sign the consent form and return it to your school. You should return the consent form even if you’re not going to have the vaccine.
We recommend you get agreement from your parent or carer, but it isn’t always necessary.
The MMR vaccine is given in 2 doses and helps protect against measles, mumps and rubella. Find out more about the vaccine, and when and where to get it.
The MMR vaccine helps to protect people against measles, mumps and rubella. It’s sometimes also offered to adults who missed their childhood immunisations.
Measles, mumps and rubella are highly infectious diseases. They can cause serious medical complications.
A high number of people in Scotland have had the MMR vaccine. This means there’s been a big reduction in the number of people catching these diseases.
All babies and children in Scotland are eligible for the MMR vaccine.
They’ll be offered the MMR vaccine in 2 doses:
Although normally given at these times, if it’s missed, it can be given at any age.
Some young people and adults who missed out on their MMR vaccine may also be eligible, like those who are a planning a pregnancy. If you didn’t have 2 doses of the MMR vaccine as a child, you can contact your local NHS immunisation team to discuss your eligibility.
If you / your child does not attend school or has missed vaccinations given in school, please contact the School Team listed under FAQs ‘School Team Contact Details’.
If your child is home schooled and has missed out on any vaccinations and you with them to be vaccinated. Then please ask your GP Practice to refer you to the Child Vaccination Team for this. On receipt of the referral the team will be in touch with you to arrange this.
The DTP vaccine provides protection against diphtheria, tetanus and polio. The vaccine is usually given in S3 (around 14 years old). Find out when and where to get it.
Immunisation (vaccination) information in other languages and formats
The DTP vaccine protects against diphtheria, tetanus and polio. These are serious diseases.
You need a total of 5 doses of the diphtheria, tetanus and polio vaccine to build up immunity and give you longer-term protection.
You should have had:
You should have the fifth dose in S3 (around 14 years old).
Diphtheria is a serious disease that usually begins with a sore throat. It can quickly cause breathing problems. It can also damage the heart and nervous system, and in severe cases, can kill. Diphtheria is passed from person to person through close contact.
Before the diphtheria vaccine was introduced in the UK, there were up to 70,000 cases of diphtheria a year. These caused around 5,000 deaths.
Tetanus is a painful disease affecting the nervous system that can lead to:
It’s caused by germs found in soil and manure getting into the body through open cuts or burns.
Tetanus can’t be passed from person to person.
Polio is a virus that attacks the nervous system and can cause permanent paralysis of muscles. If it affects the chest muscles or the brain, polio can kill. The polio virus is usually spread from person to person or by swallowing contaminated food or water.
Before the polio vaccine was introduced, there were as many as 8,000 cases in the UK during the polio epidemic.
All young people in S3 (around 14 years old) are eligible for the vaccination. This is part of their routine immunisation schedule.
The REVAXIS vaccine is routinely used in Scotland.
The DTP vaccine is not a live vaccine. It cannot cause the diseases it protects against.
The DTP vaccine is the safest and most effective way to protect against serious diseases.
You’ll be offered the DTP vaccine when you’re in S3 (around 14 years of age) at school. Vaccines are given by your local NHS immunisation team. Your school will tell you when vaccination sessions are taking place.
Find out more about the vaccinations you’ll be offered at school
If you have any questions on the day, you can speak to the person giving you the vaccine.
If you / your child does not attend school or has missed vaccinations given in school, please contact the School Team listed under FAQs ‘School Team Contact Details’.
If your child is home schooled and has missed out on any vaccinations and you with them to be vaccinated. Then please ask your GP Practice to refer you to the Child Vaccination Team for this. On receipt of the referral the team will be in touch with you to arrange this.
The meningitis ACWY (MenACWY) vaccine helps protect against meningitis and septicaemia (blood poisoning). Find out more about the MenACWY vaccine, and when and where to get it.
Immunisation (vaccination) information in other languages and formats
The meningitis ACWY (MenACWY) vaccine helps protect against meningitis and septicaemia (blood poisoning), which are caused by meningococcal bacteria A, C, W and Y.
Young people have a higher risk of getting meningococcal disease. You’ll be offered immunisation to protect yourself and others around you.
Meningitis and septicaemia are very serious diseases. They can cause permanent disability and death. The symptoms can come on quickly.
The MenACWY vaccine is routinely offered to all young people in S3 (around 14 years of age). If you’re over 14 and not already immunised, you may also be offered the vaccine.
You should not have some vaccines if you’ve had a confirmed anaphylactic shock (serious allergic reaction) to:
The following vaccines are routinely used in Scotland:
The MenACWY vaccine is highly effective at protecting against the serious infections caused by meningococcal bacteria A, C, W and Y.
The MenACWY vaccine is not a live vaccine. It cannot cause meningitis.
The MenACWY vaccine is the safest and most effective way to protect against meningococcal A, C, W and Y.
Vaccines are given by your local NHS immunisation team. Your school will tell you when vaccination sessions are taking place.
Find out more about the vaccinations you’ll be offered at school
If you have any questions on the day, you can speak to the person giving you the vaccine.
If you missed your vaccination at school
If you missed your MenACWY vaccination, there will be further opportunities to get it. For example, you may be offered a rescheduled vaccination appointment next year.
If you’re unsure if you’ve missed any other vaccines, you should first check your red book. If you do not have a red book, or it has gone missing, you can check with your local NHS immunisation team
Young people not in mainstream education
You’re also eligible for the MenACWY vaccine if you’re:
If you / your child does not attend school or has missed vaccinations given in school, please contact the School Team listed under FAQs ‘School Team Contact Details’.
If your child is home schooled and has missed out on any vaccinations and you with them to be vaccinated. Then please ask your GP Practice to refer you to the Child Vaccination Team for this. On receipt of the referral the team will be in touch with you to arrange this.
Students
You may be eligible for the MenACWY vaccination if you:
You should contact your local NHS immunisation team. They’ll advise you if it’s clinically appropriate for you to have the vaccine.
You may not be eligible for the MenACWY vaccination if you’re from outside Scotland (including other parts of the UK). You should arrange to get your vaccine before travelling to Scotland. There’s no guarantee the vaccine will be available to you after arriving in Scotland.
NHS Scotland recommends eligible children should get the flu vaccine to help protect them from influenza (flu).
Flu (influenza) is a common infectious respiratory virus. Symptoms may include a fever, a cough, a headache, and tiredness.
Flu can be serious. Even healthy children can become seriously ill from flu. In some cases flu can lead to complications. These can include bronchitis, pneumonia, painful middle-ear infection, vomiting, diarrhoea. In the worst cases, flu can lead to disability and even death.
Flu can be even more serious for people with health conditions such as:
Flu can make health conditions worse.
The flu vaccine will reduce the risk of your child getting or spreading flu to friends and family who are at greater risk from flu. For example, grandparents or people with health conditions. It’ll also help prevent your child getting sick with flu and needing time off school or nursery.
Children aged 6 months to 2 years will be given the injectable flu vaccine.
All medicines, including vaccines, are tested for safety and effectiveness before they’re allowed to be used.
Once they’re in use, the safety of vaccines continues to be monitored by the Medicines and Healthcare products Regulatory Agency (MHRA).
The nasal spray flu vaccine has been used since 2014 and has a good safety record. Millions of doses of the vaccine have been given to children in the UK.
The annual vaccine offers protection against the most common types of flu virus that are around each winter. The flu vaccine should start to protect most children about 10 to 14 days after they receive their vaccination.
In previous years, the flu vaccine has worked very well, providing protection against flu. It has also reduced the chance of spreading flu into the wider community.
NHS Scotland is offering the coronavirus (COVID-19) vaccine to children aged 6 months to 11 years at higher risk of coronavirus this spring.
To be invited for vaccination this spring, your child must have a weakened immune system and be aged 6 months to 11 years on 31 March 2024 (born on or after 1 April 2012 and before 1 October 2023).
Getting the vaccine will help to protect your child against coronavirus. The vaccine helps to build up immunity to coronavirus, so the body can fight it off more easily. If your child is vaccinated, they are much less likely to get seriously ill from coronavirus or need to go to hospital.
Infants and young children with underlying health conditions are 7 times more likely to be admitted to paediatric intensive care units with severe coronavirus, compared to those without underlying health conditions.
NHS Scotland is offering a coronavirus vaccine to children at higher risk to help protect them this spring. It’s important to keep up to date with the coronavirus vaccines your child is offered.
NHS Scotland recommends coming forward every time your child is invited to keep their protection topped up.
NHS Scotland will only use a vaccine if it meets the required standards of safety and effectiveness. All medicines, including vaccines, are tested for safety and effectiveness before they’re allowed to be used. The Medicines and Healthcare products Regulatory Agency (MHRA) assesses all the data and also ensures a vaccine works and that all the necessary trials and checks have been completed.
There are very few people who cannot have the vaccine. If your child has had a confirmed severe allergic reaction (anaphylaxis) to any of the vaccine ingredients or a previous dose of the same vaccine, you should seek advice from your health professional before your child has the vaccine.
The vaccine is not a live vaccine and does not contain any animal products or egg.
More information about the vaccines offered, including vaccine ingredients, is available in the manufacturer patient information leaflets.
Read the coronavirus vaccine patient information leaflet for 6 months to 4 years:
NHS Scotland recommends eligible children should get the flu vaccine to help protect them from influenza (flu).
The flu vaccine is available between September and March.
Flu (influenza) is a common infectious respiratory virus. Symptoms may include a fever, a cough, a headache, and tiredness.
The flu vaccine is offered as a painless nasal spray to almost all children. It cannot give the child flu but starts to provide protection against flu within 10-14 days. The nasal spray offers the best possible protection for children and young people and can also stop flu spreading to family, friends and others, especially those most at risk of becoming seriously ill with flu. Children aged 2 to 5 are being offered vaccination from the start of the programme to ensure they receive the earliest protection and prevent the virus spreading.
Flu can be serious. Even healthy children can become seriously ill from flu. In some cases flu can lead to complications. These can include bronchitis, pneumonia, painful middle-ear infection, vomiting, diarrhoea. In the worst cases, flu can lead to disability and even death.
Flu can be even more serious for people with health conditions such as:
Flu can make health conditions worse.
The flu vaccine will reduce the risk of your child getting or spreading flu to friends and family who are at greater risk from flu. For example, grandparents or people with health conditions. It’ll also help prevent your child getting sick with flu and needing time off school or nursery.
In Scotland, children aged 2 to 17 will usually be given the nasal spray flu vaccine. It’s quick and painless and there’s no need to sniff or inhale the vaccine. It’ll just feel like a tickle in their nose.
Children aged 2 to 17 years who cannot receive the nasal spray vaccine will receive the injectable flu vaccine.
All medicines, including vaccines, are tested for safety and effectiveness before they’re allowed to be used.
Once they’re in use, the safety of vaccines continues to be monitored by the Medicines and Healthcare products Regulatory Agency (MHRA).
The nasal spray flu vaccine has been used since 2014 and has a good safety record. Millions of doses of the vaccine have been given to children in the UK.
The annual vaccine offers protection against the most common types of flu virus that are around each winter. The flu vaccine should start to protect most children about 10 to 14 days after they receive their vaccination.
In previous years, the flu vaccine has worked very well, providing protection against flu. It has also reduced the chance of spreading flu into the wider community.
NHS Scotland recommends eligible children should get the flu vaccine to help protect them from influenza (flu).
The flu vaccine is available between September and March.
Flu (influenza) is a common infectious respiratory virus. Symptoms may include a fever, a cough, a headache, and tiredness.
The flu vaccine is offered as a painless nasal spray to almost all children. It cannot give the child flu but starts to provide protection against flu within 10-14 days. The nasal spray offers the best possible protection for children and young people and can also stop flu spreading to family, friends and others, especially those most at risk of becoming seriously ill with flu.
Consent forms and further information will be sent home to parents and carers of school children on return to school. Secondary pupils can self-consent but are encouraged to speak to a parent or carer first. All primary and secondary school pupils with consent to be given the flu vaccine nasal spray will receive this at school starting in early September through to December 2024.
Flu can be serious. Even healthy children can become seriously ill from flu. In some cases flu can lead to complications. These can include bronchitis, pneumonia, painful middle-ear infection, vomiting, diarrhoea. In the worst cases, flu can lead to disability and even death.
Flu can be even more serious for people with health conditions such as:
Flu can make health conditions worse.
The flu vaccine will reduce the risk of your child getting or spreading flu to friends and family who are at greater risk from flu. For example, grandparents or people with health conditions. It’ll also help prevent your child getting sick with flu and needing time off school or nursery.
In Scotland, children aged 2 to 17 will usually be given the nasal spray flu vaccine. It’s quick and painless and there’s no need to sniff or inhale the vaccine. It’ll just feel like a tickle in their nose.
Children aged 2 to 17 years who cannot receive the nasal spray vaccine will receive the injectable flu vaccine.
Children aged 6 months to 2 years will be given the injectable flu vaccine.
All medicines, including vaccines, are tested for safety and effectiveness before they’re allowed to be used.
Once they’re in use, the safety of vaccines continues to be monitored by the Medicines and Healthcare products Regulatory Agency (MHRA).
The nasal spray flu vaccine has been used since 2014 and has a good safety record. Millions of doses of the vaccine have been given to children in the UK.
The annual vaccine offers protection against the most common types of flu virus that are around each winter. The flu vaccine should start to protect most children about 10 to 14 days after they receive their vaccination.
In previous years, the flu vaccine has worked very well, providing protection against flu. It has also reduced the chance of spreading flu into the wider community.
Where clinics take place
Vaccinations are typically given in schools during term time. NHS GGC work with schools to communicate programme dates.
Before clinics take place, consent forms and vaccination information will be handed out to pupils at school for review at home then return to school.
If you / your child does not attend school or has missed vaccinations given in school, please contact the School Team listed under FAQs ‘School Team Contact Details’.
On the day
Pupils will usually attend clinics in the school hall or social space, class by class throughout the day.
About the programme
Immunisation is the safest and most effective way of protecting young people against serious diseases.
School-aged children are routinely vaccinated against:
The flu vaccine is offered as a painless nasal spray to almost all children. It cannot give the child flu but starts to provide protection against flu within 10-14 days. The nasal spray offers the best possible protection for children and young people and can also stop flu spreading to family, friends and others, especially those most at risk of becoming seriously ill with flu.
Consent forms and further information will be sent home to parents and carers of school children on return to school. Secondary pupils can self-consent but are encouraged to speak to a parent or carer first. All primary and secondary school pupils with consent to be given the flu vaccine nasal spray will receive this at school starting in early September through to December 2024.
https://www.nhsinform.scot/vaccineconsentyoungpeople
For details of the schedule of vaccinations in Scotland by age, please refer to NHS Inform.
Where clinics take place
Vaccinations are typically given in schools during term time. NHS GGC work with schools to communicate programme dates.
Before clinics take place, consent forms and vaccination information will be handed out to pupils at school for review at home then return to school.
If you / your child does not attend school or has missed vaccinations given in school, please contact the School Team listed under FAQs ‘School Team Contact Details’.
On the day
Pupils will usually attend clinics in the school hall or social space, class by class throughout the day.
Please contact your GP
Please see team contact details below:
Glasgow South/East Renfrewshire
Phone Number: 0141 577 7774 (voicemail service is available)
Opening Times: Monday -Thursday 08.30am – 16.30pm and Friday – 08.30am – 16.00pm
Health Centres: Castlemilk, Eastwood, Govanhill, Gorbals, Govanhill (EU), Pollock, Shields Centre, Elderpark, Thornliebank, Barrhead
North East/East Dunbartonshire
Phone Number: 0141 531 6635 (voicemail service is available)
Opening Times: Monday -Thursday 08.30am – 16.30pm and Friday – 08.30am – 16.00pm
Health Centres: Springburn, Kirkintilloch, Stobhill, Milngavie, Baillieston, Shettleston, Bridgeton, Townhead, Easterhouse
North West/West Dunbartonshire
Phone Number: 0141 211 6142 (voicemail service is available)
Opening Times: Monday -Thursday 08.30am – 16.30pm and Friday – 08.30am – 16.00pm
Health Centres: Dumbarton, Vale of Leven, Maryhill, Woodside, Possilpark, Community Centre for Health (CCFH), Plean Street, Drumchapel, Clydebank
Renfrewshire/Inverclyde
Phone Number: 0141 201 1056 (voicemail service is available)
Opening Times: Monday -Thursday 08.30am – 16.30pm and Friday – 08.30am – 16.00pm
Health Centres: Greenock, Port Glasgow, Johnstone, Linwood, Renfrew, Foxbar Clinic, Northcroft, Tannahill Centre, Erskine
Please see team contact details below:
Glasgow South/East Renfrewshire
Phone Number: 0141 577 7767 (voicemail service is available)
Opening Times: Monday -Thursday 08.30am – 16.30pm and Friday – 08.30am – 16.00pm
North East/East Dunbartonshire
Phone Number: 0141 232 9838 (voicemail service is available)
Opening Times: Monday -Thursday 08.30am – 16.30pm and Friday – 08.30am – 16.00pm
North West/West Dunbartonshire
Phone Number: 0141 232 9202 (voicemail service is available)
Opening Times: Monday -Thursday 08.30am – 16.30pm and Friday – 08.30am – 16.00pm
Renfrewshire/Inverclyde
Phone Number: 0141 314 0513 (voicemail service is available)
Opening Times: Monday -Thursday 08.30am – 16.30pm and Friday – 08.30am – 16.00pm
When you or someone you care about becomes ill, life can become very stressful. That is why we think it is so important for people to talk to each other and make plans before this happens.
To help people plan more, and stress less, we have created a toolkit of resources that we hope will be useful. This includes the recorded information session below and checklists to help you get organised, as well as a plan to work out how you’d get home from hospital. We also look at some of the legal process and support that is available for those who care for you.
Even if you and those you support are perfectly healthy just now, you can still use these tools to help plan for the future!
We have recorded the “Plan More, Stress Less” session below for anyone interested in getting started with planning ahead. In this session we talk about what paperwork we can complete before a crisis arises, what actually happens when someone goes into hospital and how we can all work together to plan for a safe and timely discharge.
Watch the recording here:
Alongside this video we have created two resources which anyone can use to help them plan for any future hospital admission. This could be a planned admission, for example if someone is going to hospital for an operation or to have some tests. However these resources can also be useful if someone needs to go to hospital in an emergency.
If you have any questions or feedback about these resources please email ggc.HomeFirst@nhs.scot
This checklist will help you think about all the different forms which you can complete just now that would be useful if you were ever in hospital. This includes things like a Future Care Plan and a Power of Attorney.
This resources lets you and the people who support you, think about what might need to happen in order to get you home from hospital in a safe and timely manner. This includes thinking about who could collect you from hospital and where you might need to live if you need some extra support for a short time or on a more permanent basis.
Welcome to the Ward / Department posters are in place at all ward/department entrances to provide at-a-glance essential information for visitors to the area.
Please send all requests for additional or replacement posters to: ggc.medical.illustrationgri@nhs.scot.
Be sure to include your local cost-code for all posters ordered.
To arrange to have new or updated SCN pictures taken, please contact Medical Illustration direct at:
No. Welcome to the Ward / Department posters represent current visiting arrangements, as per the Scottish Government Visiting guidance.
Please contact the Person Centred Health and Care Team at ggc.person.centred@nhs.scot with any further questions, feedback or comments.
HENRY provides a wide range of support for families from pregnancy to age 12 including workshops, programmes, resources and online help. Support for families is underpinned by the HENRY approach to supporting behaviour change which helps parents gain confidence, knowledge and skills they need to help the whole family adopt a healthier, happier lifestyle and to give their children a great start in life.
Healthy Families Right from the Start encourages parents and carers to adopt a whole family approach. The programme covers:
Healthy Families Growing Up includes more age-relevant topics such as body image, the influence of peers and family negotiations.
The programme covers:
These stand-alone workshops provide key information, confidence-building and peer support for families and can also act as “taster sessions” for families who may be interested in attending the Henry programmes. There are 7 topic specific workshops:
Families living in Greater Glasgow and Clyde can now access HENRY for support with:
HENRY is a holistic family programme and is not a specialist intervention, however families who have children with complex needs may still benefit from attending.
If you are working with children and families you can refer families to HENRY using the Health Professional Referral Form.
If the family lives in Glasgow Northeast complete this referral form.
If the family lives in any of the areas listed below, complete this referral form.
To find out more about what HENRY has to offer, please visit the HENRY website or watch the video below.
HENRY – Healthy Start, Brighter Future