Are you having trouble sleeping?
Many people experience sleep difficulties at some time in their lives. In fact, it is normal to feel that sometimes you have not slept well. It might be that you felt it has taken a long time to fall asleep or maybe you felt you tossed and turned all night. A familiar feeling that can leave us feeling a bit tired and worn out the next day.
For some people, this experience of poor sleep or dissatisfaction with their sleep can last a long time. Sometimes people might describe themselves or their partner as having insomnia. Let’s have a closer look at what would be considered a normal sleep pattern and when we might consider someone to have a problem with sleep or insomnia. In addition, we will take a brief look at some other medical conditions that can cause sleep disruption. If you think you might have any one of these conditions, you should contact your GP.
More Information
What is normal sleep?
Individuals vary greatly in terms of how much sleep they need however as a general rule, there are patterns that fluctuate as we age. The amount of sleep we need in general reduces as we get older and the typical adult sleeps between 7-8 hours per night and then in later life, sleep can become less consolidated at night time and on average older adults sleep for 6-6 ½ hours per night with some napping throughout the day.
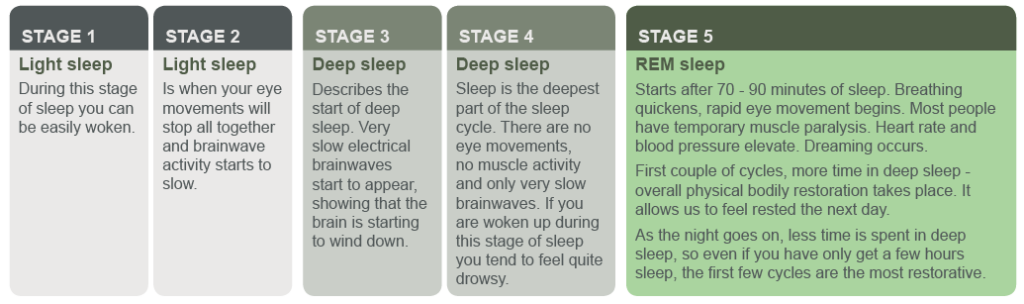
So, we now know that on average, all being well, an adult should be sleeping for approximately 7-8 hours per day. Let’s look at what happens during that time asleep. Using specialist equipment that measures brain and muscle activity, researchers and scientists have been able to identify sleep cycles that are made up of 5 distinct stages of sleep; stages 1 to 4 and rapid eye movement (REM) sleep. A sleep cycle will last between 90 and 110 minutes and we tend to go through 4 to 5 sleep cycles per night.
What is insomnia?
So far we have been looking at what sleep is but what about when we don’t sleep. What is going on?
Occasional sleep disturbance is common and quite a normal experience familiar to us all. Everyone experiences difficulty getting to sleep or staying asleep at some time in their lives. This often occurs at times of change or times of stress. These problems usually sort themselves out and end up being short-lived, and once the stressor goes, so do the sleep problems. However, we know from studies that examine the occurrence of insomnia in the population, that about 10% of adults, that is 1 in 10 people, experience persistent sleep problems, and this can be as high as 1 in 5 (20%) in people over 65 years of age.
A widely accepted definition is supplied by the American Sleep Disorders Association (ASDA, 1997):
Insomnia is a condition where you have problems getting to sleep or staying asleep for 3 or more nights per week and persisting for at least 6 months. There might also be daytime mood and performance effects.
Source: based on the revised International Classification of Sleep Disorders, ASDA, 1997
People with insomnia often experience:
- Difficulty falling asleep
- Difficulty staying asleep
- Frequent nighttime awakenings
- Feeling very tired the next day.
The definition from the latest Diagnostic and Statistical Manual (American Psychiatric Society) is similar: this is the manual used by clinicians and researchers to diagnose and classify mental disorders. In the fifth edition, published in May 2013 (DSM-5), insomnia disorder is defined as a combination of both dissatisfaction with sleep and a significant negative impact on daytime functioning.
Dissatisfaction with sleep is further defined as difficulty initiating and/or maintaining sleep or non-restorative sleep, on at least three nights per week for at least 3 months, despite adequate opportunity to sleep. Negative daytime impacts can include significant fatigue, sleepiness, poor concentration, low mood, or impaired ability to perform social, occupational or caregiving responsibilities.
If you are interested in finding out more about your sleep difficulties NHS Choices has more information
Sleep Problems, Insomnia and other Sleep Disorders
Some insomnia is a natural consequence of a stressful period in a person’s life or leading up to a stressful event such as a job interview or making a presentation. Usually, once these events pass, sleep returns to normal.
On occasion, poor sleep can continue, and this can start a cycle where a person starts to worry about not sleeping. This can result in anxiety that makes it even more difficult to get to sleep or stay asleep. The more you worry, the harder it is to sleep.
So there are different drivers to Insomnia. Some are to do with how we cope with stressful situations, and others are to do with worry about the Insomnia itself.
Sleep Disorders other than insomnia
When talking about Insomnia, we are not talking about medical conditions that cause sleep problems. Advice should be sought from a medical practitioner in such cases. There are different types of sleep problems, and these are described below:
Circadian Disorder
Delayed sleep phase syndrome –this involves the experience of staying awake until late at night with problems initiating sleep and with waking in the morning. People with this feel sleepy even when waking at normal rising times, and feel that they sleep better when they go to bed late and get out of bed later in the morning.
Advanced sleep phase syndrome –this involves the experience of feeling sleepy in the evening and finding it difficult to stay awake until a normal bedtime. Typically people experience early morning wakening and sleep better when they go to bed very early and get up out of bed very early.
Sleep-related breathing disorder
Obstructive sleep apnoea – commonly snoring loudly, breathing can be irregular or have ‘pauses’, and sleep is broken with periods of brief wakening. People with this often experience feeling sleepy during the daytime and might have difficulty with low mood. This breathing problem can be linked to being overweight.
Agitated movement of legs and limbs
Periodic limb movement disorder –this is characterised by jerky movements of the limbs that interrupt sleep or repetitive movements during sleep. This can lead to tiredness during the daytime.
Restless leg syndrome –this is involuntary movement of the legs during sleep and this can also be associated with insomnia and/or being tired during the daytime.
Parasomnias (abnormal sleep behaviour)
- Sleepwalking – this typically occurs during deep sleep and involves actions such as walking whilst asleep. As the person is in deep sleep during the behaviour, they are difficult to wake up and they do not usually recall the behaviour.
- Sleeptalking – this can happen throughout stages of sleep and involves producing speech or speech-like sounds whilst asleep.
- Night terrors – this refers to experiencing, whilst asleep, extremely upsetting emotions that are difficult to waken from.
- Nightmares – these are dreams that are distressing and usually wake you up.
Narcolepsy
- Sleep attacks – unexpected and uncontrollable bouts of sleep during the daytime.
- Hypersomnia – excessive sleepiness and extended sleep.
- Cataplexy – sudden loss of muscle tone in response to emotion.
- Sleep paralysis – inability to move especially on waking from sleep.
Sleep disorders associated with medical or psychiatric disorders
Many medical disorders have sleep problems associated with them. Mental health problems can also affect sleep patterns and quality. These should also, therefore, be considered when you encounter sleep problems.
A psychological approach to understanding insomnia
A diagnosis is often helpful. It helps us to have a name for what is causing us distress. It can also help us think about what we might need to do to get better.
A psychological understanding of a problem is also very helpful. Psychologists use a process called formulation to help develop a detailed understanding of a person’s difficulty. A formulation will typically describe predisposing, precipitating and perpetuating factors.
Predisposing factors
These factors refer to those things in life that might have made you vulnerable to developing a particular problem. In relation to insomnia, this could include having always been a poor sleeper, having a condition such as ADHD or having a family history of poor sleep.
Can you think of any predisposing factors you may have that might make you more likely to be a poor sleeper?
Precipitating factors
This refers to “triggers” – what was happening at the time that contributed to you developing a problem. In relation to insomnia, examples could include a house move, being diagnosed with a health condition or family/work-related stress. A study published in 2004 found that 60% of patients with insomnia could identify a trigger for their sleep disturbance, and these tended to be around family, work/school and health (Bastien et al. 2004).
Take a moment to think if there are any changes in your life, or big events, that started around the time of your sleep problems. These might be ’precipitating factors’.
Perpetuating factors
This refers to those factors that keep the problem going or exacerbate it. For example, sometimes when we have a bad nights sleep, we might worry about it and this worry makes if difficult to get to sleep the next night. We might then have thoughts that cause anxiety such as “I will never get to sleep”- such thinking, causes anxiety that maintains sleep difficulties. Alternatively, we might develop some coping behaviours such as having a nap throughout the day or drinking alcohol at night. These coping behaviours can actually keep the problem going as they disrupt the sleep routine. Perpetuating factors, therefore, keep the problem going, even after the initial trigger might have passed.
Have you noticed that you have become more worried about getting enough sleep? What are your thoughts before bedtime? You might have changed some routines or be napping during the day to ‘catch up’. These might be ‘perpetuating factors’ that are maintaining your insomnia.
From Formulation to Intervention
Okay, so now you might have an idea as to what has caused your sleep problems but what can you do about it? Understanding sleep difficulties, keeping in you’re your own predisposing, precipitating and perpetuating factors can help you understand how to get better using an intervention called Cognitive Behavioural Therapy. This type of therapy is considered to be the gold standard treatment for insomnia and research has shown this to be the case. Typically, CBT focuses on the perpetuating factors; those thought processes and behaviours that might be maintaining the problem or making it worse.
The Bed-Sleep connection
When we are sleeping well, we have a strong bed-sleep connection. This means that we associate being in bed with sleeping. The very thought of going to bed induces feelings of relaxation and sleepiness. We start to engage in our sleep routines, sleepiness increases, we climb into bed and fairly quickly we fall asleep. The bed acts as a ’cue’ to sleep. As described above, some people may have difficulties with sleep that has weakened the strength of the bed-sleep connection. It could be that you have always been someone that does not sleep well. Or perhaps you grew up with parents that rarely slept well. If this is the case you might not have a strong bed-sleep connection. For you, the notion of bed does not induce sleepiness as powerfully as it does for others. Or, perhaps you have always been a good sleeper, however, something happened in your life that triggered poor sleep- you got a new job for example and this caused some anxiety. This might have lead to you lying in bed awake, feeling anxious, tossing and turning throughout the night. As this continues, the bed-sleep connection weakens. You start to associate the bed with lying awake and feeling anxious rather than being asleep. A goal of cognitive behavioural therapy for insomnia is to strengthen this bed-sleep connection. In this web-page, you will find various techniques to help you to establish this.
What helps – Things you can do to improve your sleep
Sleep Diary
Keeping a sleep diary can be a really helpful strategy that can help you develop a greater awareness of your sleep. The better you understand your sleep and it’s patterns and variations across the week, the more equipped you will be to address your sleep difficulties. Keeping a sleep diary can also reduce distress about your sleep. At times we might think “I never sleep” and this can make us feel frustrated and upset. This leads to anxiety about sleep which in itself makes the sleep problem worse! Looking at our sleep diary can help us keep our thinking in check and remind us of the nights when we slept better. Your sleep diary does not need to be precise so don’t worry about clock checking- it is just to give you a rough estimation of how you slept the night before. Try and complete it within the first hour of waking.
Sleep Hygiene
By changing some of our lifestyle habits and our environment, we can make significant improvements to our sleep. This is what sleep hygiene refers to. It is sorting out the basics of good sleep. There are lots of practical things you can do to help you get a better night sleep.
Caffeine
Caffeine is a stimulant drug; this means that it perks you up and makes you feel more alert. Caffeine can be found in drinks (e.g. coffee, tea and cola), food (e.g. chocolate) and medications. Many people use caffeine to get going in the morning or to waken up in the evening. Anyone who has had a difficult nights sleep will relate to wanting a strong coffee to get going! The problem is, this stimulant can also keep you awake at night time, just when you should be winding down and going to bed. The effect of caffeine can last for many hours, therefore, it is recommended to avoid it for 4-6 hours before bedtime.
Nicotine
This is another stimulant drug – it stimulates the nervous system. This means that rather than relaxing our bodies, it actually perks us up. This can have a negative impact on sleep, keeping us awake rather than helping us to fall asleep. The addictive nature of nicotine can further disrupt the sleep process as cravings can wake the body up. Some smokers might be in the habit of waking up throughout the night to smoke, disrupting a healthy sleep routine. If you are a smoker and you are experiencing sleep problems, it would be a good idea to try and cut down on how much you smoke and avoid smoking throughout the night. This is easier said than done. There is more information on stopping smoking.
Alcohol
Alcohol is a depressant drug and unlike a stimulant, this slows the body down. Some people even report that it “helps” them sleep. Unfortunately this is not the case. Whilst alcohol can induce sleepiness and make it more likely that you will fall into a deep sleep, as the alcohol gets absorbed by your body, alcohol withdrawal starts that can cause you to waken or move into a lighter stage of sleep. Side effects of alcohol include dehydration and the need to urinate and both of these things can cause you to wake up. So, although alcohol might help you fall asleep, the sleep quality is poor and not restorative. It is recommended that alcohol should be avoided for 4 hours before bedtime.
Diet
Both hunger or overeating at bedtime can disrupt sleep. If you feel hungry before bed, a light snack can help and stop feelings of hunger causing wakefulness. However, avoid a large meal before bedtime as the body has to work hard digesting food and this can disrupt sleep. Also, food gives energy so choose a non-sugary snack to avoid a “sugar rush” at night time.
Some people have reported that a warm milky or malty drink at bedtime can help promote sleep. Avoid caffeinated drinks like tea/coffee or coke!
If you are someone who wakens in the night and heads to the kitchen for a snack, try and cut this out. The body can start to expect food in the middle of the night and this may increase night time awakenings.
Exercise
Physical fitness is associated with better sleep. A great way to improve sleep is to try and fit in some physical exercise to your day. People should aim to do 20 – 30 minutes of physical exercise, at least three times week. This doesn’t mean you have to take up going to the gym, you could go for a walk, jog or a swim. Or what about doing something with a friend like a game of tennis or badminton? Introducing exercise to your day can help you get that good night sleep, however, avoid doing it too close to bedtime as that can waken you up! Try and fit it in before the evening.
In addition to making small changes to our lifestyle, making changes to our bedtime routine and the sleep environment can also help improve your sleep. Let’s have a look at what you can do.
Noise
Noise can disrupt our sleep: sudden banging, a baby crying or a car horn beeping can all waken us up, even from a deep sleep. However, we can also get used to noises in the background such as light traffic and the wind. It can be worth having a look and a listen in your bedroom and trying to identify any noises that could be keeping you awake or disrupting your sleep. Does the boiler kick in at 3am? Is there something that beeps in the night? Do your heaters creak as the heating comes on? Do you have a partner that snores? Can you make changes to this to ensure a silent night? For example, some people find that wearing earplugs help. There might be some noises that you can’t control, but trying out different relaxation techniques (see relevant section) can help.
Room temperature
Ideally your room should be around about 18 degrees Celsius. A room that is too hot or too cold can significantly disrupt sleep so get a thermometer and see if this helps.
Body Temperature
People who often report feeling too hot are more likely to have sleep difficulties. Although many people like to have a bath before bed to help them sleep, if this raises your body temperature, it might actually make sleep more difficult. Having said that, a bath can be a nice part of a bedtime routine. Make sure and have it at least an hour before bed so that your body temperature returns to normal. A very heavy duvet or thick pyjamas might also raise your body temperature so consider these factors when making changes to your sleep environment.
Air Quality
Fresh air can help promote sleep. It might be an idea to open your window for a while before bed to let in some fresh air. Of course, bear in mind the time of year and temperature!
Lighting
Natural light levels influence the production of melatonin. This is a hormone that controls our body clock. When it is dark, melatonin production increases causing sleepiness and as natural light creeps in during the morning, this decreases the production of melatonin, reducing sleepiness. It is therefore important to consider light when making changes to your sleep environment. Ensure curtains are drawn and that as much light is shut out as possible. If you have thin curtains, putting a blanket across your window might help or alternatively consider wearing an eye mask. Keep artificial light to a minimum or not at all during the night time. Also, avoid looking at tablet/laptop devices before bed as the light that comes from these objects can inhibit the production of melatonin which can get in the way of feeling sleepy.
Bed Comfort
Feeling discomfort throughout the night is going to disrupt your sleep. Consider the comfort of your mattress, pillow and bedding. Is the mattress the right size, is it too hard or too soft? What about your pillow? Is it too thick or too thin, do you need two pillows or none at all? Is your bedding clean and comfortable? It is worth experimenting a bit here to find out what suits your own preferences best.
Make a list of some goals that you are going to put in place with regards to sleep hygiene. What changes could you make to your lifestyle and to your environment to help you get a better nights sleep?
Developing a Sleep Routine and Unwinding Before Bed
It would be unrealistic to think that you can go to bed at any time and simply fall asleep. A good period of winding down can help the body and mind prepare for sleep. A consistent sleep routine helps create cues that lead to the body and mind winding down ready for bed. We do this for babies, don’t we? Many people get their babes into an evening routine of “bath, bottle then bed” and we can see how such a consistent routine prepare the infant for bed. Adults need this too! It is a good idea to start your sleep routine a good 60 to 90 minutes before going to bed. Try to first slow down and stop your activities and work and switch to relaxing activities. Adjust the lighting so that it is less bright. Perhaps have a bath before getting a light snack and having a read of a book. Consider what you find relaxing and try to implement that into your day here. Then, once you are feeling sleepy, prepare for bed (e.g. lights out, lock doors, brush teeth).
Relaxation
Being in a relaxed state before going to bed is certainly helpful. Many people who have sleep difficulties find this difficult: as sleep problems develop, people can become anxious as they get ready for bed, wondering if they will manage to sleep that night. If this is you, learning some relaxation techniques could be helpful. Relaxation does not always come automatically but it can be learned. There are many things that we do to relax and some of these are fairly active relaxation pursuits such as exercise. Such activities use up energy leaving us feeling relaxed afterwards. Other types of relaxation are more about easing the body and mind, slowing down and letting go. Activities of this type could include reading a book or having a bath. It might be helpful to write a list of things that you can do to help cause a state of relaxation and introduce these to your day or pre-bedtime routine.
Relaxation Techniques
In addition to these activities some people find that engaging in a relaxation technique, can help facilitate a state of relation and sleepiness. Please follow the links below to access relaxation techniques
Progressive Muscle Relaxation
Information on progressive muscle relaxation
Mindful breathing
Information on mindful breathing
Meditation
Information on meditation
These relaxation techniques can help to relax our bodies and our minds. There are other strategies that you can use to help you to learn to manage difficult thoughts and/or worries. Many people find that they can’t sleep because their mind does not stop. You might be worrying about what has happened that day, or what you need to do the next day. Try some of these techniques to help manage your thoughts/worries.
Putting the Day to Rest
Do you lie in bed at night and remember all the things you should have done but didn’t. Or suddenly remember something you need to do the next day? A helpful tool for this type of anxiety is to spend approximately 20 minutes in the evening thinking about your day and what is happening the next day and writing anything down that you need to do. Professor Colin Espie, an International Sleep Expert calls this putting the day to rest. He recommends following to help put the day to rest.
- Set aside 20 minutes in the early evening, at the same time each night
- Sit somewhere where you will not be disturbed
- All you need is a notebook, a diary and a pen
- Think about what has happened during the day, how you feel it has gone
- Write down some of the main points. Put them to rest by putting it on paper. Record what you feel good about as well as what has been difficult
- Write a “to do” list
- Now think about tomorrow, what is coming up, what you are looking forward to and what is troubling you
- Write down the schedule in your diary if not done so already
- Write down anything you are unsure about and make a space in your diary for when you can find out more about it
- Use these 20 minutes to take control of what has happened and what is coming up. Close the book on the day
- As you go to bed, remember that you have dealt with all that you can and that you have put the day to rest
- Keep some paper by your bed so that if any new thoughts pop up, you can jot them down to be dealt with in the morning
Thought Blocking
Some people find that their mind really races at night time, flitting from thought to thought. Putting the day to rest can really help. Another technique to employ when in bed is “thought blocking”. This is a technique that stops you thinking of the annoying fleeting thoughts. What you do is repeat the word “the” every 2 seconds (say it in your head) and keep this up for about 5 minutes. This blocks out the unwanted thoughts with a word that is meaningless. It is therefore unlike to have an emotional effect and will therefore not cause arousal but rather boredom!
Paradoxical thinking
When sleep does not come, we can become really preoccupied with trying to get to sleep. The more we try and fail, the more distressed and anxious we can become and the more we try and try to sleep! With sleep, the harder you try the less likely it is that sleep will happen. One method to overcome this type of anxiety is to turn things around and actually try to stay awake. Lie in bed, keep your eyes open and say to yourself that you are going to stay awake. As you start to feel sleepy, try and think about staying awake for a few minutes longer. Turning your thinking away from trying to sleep to trying to stay awake, can reduce the preoccupation with sleep that leads to distress and wakefulness.
Re-evaluating some of your thoughts
Our thoughts can have a powerful effect on how we feel. If we are thinking negatively we can feel quite down or anxious. This, in turn, can impact upon our sleep as we develop anxiety about sleeping. Our thoughts about sleep are not always accurate and as we become anxious, out thoughts are more likely to become distorted and faulty. To check in on our thoughts and to evaluate their accuracy, it can be helpful to keep a thought diary.
Often where there is an emotion such as worry or sadness, our thoughts can become distorted, and are usually quite negative! If we write down how the thought makes us feel, and then stand back and re-evaluate that thought, we might come up with a more balanced picture.
You can use the diary below to try this. Write down your sleep thoughts and how these make you feel. Then evaluate the accuracy of that thought and see if you can write down a more balanced version of that thought. Again, consider how this new thought makes you feel. If you find this difficult, try asking someone to help you come up with a more balanced thought – this helps provide a different perspective.

Strengthening the Connection Between Bed and Sleep
As described earlier, improving that automatic connection made by the brain between bed and sleep, is an important part of overcoming sleep difficulties. By implementing many of the strategies described, you are more likely to get a good nights sleep. The more experiences you have of sleeping, the stronger your bed- sleep connection becomes. Here are some more tips to help build up that connection:
The bed should be for sleeping. Avoid spending long periods of time reading or watching TV in bed. Sexual activity is the only exception!
Go to bed when you feel sleepy-tired. If you go to bed whilst you still feel wide awake, you may find your self tossing and turning.
If you have been having sleep problems for a while, aim to spend approximately a quarter of an hour getting to sleep. If you are still awake, get up and do something relaxing. This stops you spending a lot of time being wakeful in the bed. Return to bed once you feel sleepy tired. If again, you are not asleep after a quarter of an hour, get up again! It is a good idea to prepare for this: ensure you have a nice and relaxing room to go to and have a think of what relaxing activities you might do at this time. It can feel lonely being up on your own to prepare.
Avoid napping throughout the day. The daytime is for being wakeful and night time is for sleeping. You want to ensure these associations (day-wake and night-sleep) are in place and are strengthened. Although you might want to nap, in general, this makes a sleep problem worse. It weakens the bed – sleep association and also gets in the way of building up the need for sleep throughout the day.
Living with…Insomnia
The Impact of Insomnia
Mood
Insomnia can be a very isolating condition as the effects are not clearly visible. Symptoms of fatigue, poor concentration and low mood are felt by the person, but cannot be easily identified as difficulties in the eyes of others. Friends, family or carers can be dismissive of the impact or worry that insomnia causes for the individual, and this can make them feel even worse about the condition. They can feel isolated and sometimes dismissed when others also claim they have sleep problems as well (but are referring to lesser symptoms). In addition, the period when not awake can in itself feel very lonely for the person suffering the condition, and they can be limited in what activities they can do during this period. There is evidence that shows there is a big overlap in the number of people that suffer Insomnia that also suffer depression. It is difficult to determine which might cause the other if there is a causal link at all. This remains unclear.
Relationships
Relationships can be affected too. There is sensitivity about disturbing partners/close family, and increased sensitivity or guilt. Sometimes a partner may decide to sleep in a separate room so as not disturb the other person, such is their increased self-awareness or potential to cause arguments or disagreement. These fears and feelings were borne out in the comments made in interviews with a group who had insomnia and chronic pain. You may recognise some of these sentiments:
“Well I’m very private and don’t talk about my… lack of sleep at all…except to my husband. Well they’re (other people) just ignorant and it’s okay lets just, you know, that’s fine, we’ll just go along like that…”
“Well my good friends, they will be interested to know how I’m feeling. I don’t really expect people to want to know how I’m feeling.”
“This is the first time I’ve ever spoke about it, about sleep …even when I think about friends I haven’t spoke about that in connection with pain…I don’t find it easy to speak to just everybody.”
“I used to text her (my daughter) during the night and she used to say ‘dinnae text me during the night ‘cos my phone goes off’…”
“It’s boring really. You cannae do this, you cannae do that, you cannae even shove some washing in the machine and put it on ‘cos you’re annoying your neighbours then. You cannae do nothing.”
“…my husband is blessed with a very good nature and he is an angel really. He’s very good. I do my very best to keep him in a good, amiable mood and happy so we can both manage between us.”
“Yeh, I’m frustrated because I can’t sleep and I’m shouting at my mum on the texts and then I have to say I shouldnae have said that so I say ‘sorry’ and she says ‘that’s okay, am (I’m) your mum’ but I feel terrible and I shouldnae be doing that.”
You might also look at the Mood section of this website on ways to help, such as talking to friends and family about things.
Find out more
NHS
- Information from the NHS on Sleepio
- Helpguide.org information on sleep
- NHS Choices information on sleep
Other services
There is an online Cognitive Behavioural Therapy course called Sleepio that has a growing evidence base for helping people over come sleep difficulties. It is possible to receive this online course for free by registering to take part in their research project, details are available from Sleepio and the National Sleep Foundation (USA)
Acknowledgements
Espie, C. (2010). Overcoming insomnia and sleep problems : A self-help guide using cognitive behavioral techniques. London: Constable and Robinson.
Looking after someone with…Insomnia
Those suffering insomnia can feel the symptoms of tiredness, loneliness, poor daytime functioning (concentration and motivation), and there is often low mood present too. The physical symptoms can be difficult to manage, but what can make things worse is the feeling that nobody takes their symptoms seriously, and that they are dismissed as ‘just having some sleep problems’. In reality, this can make sufferers feel not believed and affect their mood. They can feel misunderstood and isolated, even when around others.
If a loved one has Insomnia it is important to take them seriously, even if you can’t see any symptoms yourself. Direct them to this website where they can learn and identify what symptoms they have and whether this is actually insomnia, or another health condition that is behind their sleep problems.
On this Insomnia section, there are self-assessment measures they can use and even try some self-help strategies to get started with. Often simple changes to the bedroom environment or a good routine before heading to bed can make a big difference. Have a look at the other sections in this Insomnia section for some useful tips and strategies.
But remember, believing them is important. Take them seriously and show understanding. Unless you also have (or have had) Insomnia, don’t say you know what it’s like – this makes them feel like you are trivialising their problem. Say that you don’t know what it’s like, but that it sounds very hard to deal with, and that you’ll try to help them as much as you can. If you share a bed with them, don’t give them a hard time for getting up during the night or accidentally waking you. This will just make them more stressed and less likely to get to sleep. Be kind, supportive and show them you care. That can make a huge difference.
Further information for carers is available on the NHS Greater Glasgow and Clyde carers site
BSL – Sleep Disorder
NHSGG&C BSL A-Z: Mental Health – Sleep Disorder
Occasional sleep disturbance is common and quite a normal experience familiar to us all. Everyone experiences difficulty getting to sleep or staying asleep at some time in their lives. This often occurs at times of change or times of stress. Insomnia is a condition where you have problems getting to sleep or staying asleep for 3 or more nights per week and persisting for at least 6 months. There might also be daytime mood and performance effects.
People with insomnia often experience:
- Difficulty falling asleep
- Difficulty staying asleep
- Frequent night time awakenings
- Feeling very tired the next day
Please note that this video is from a range of BSL videos published by NHS Greater Glasgow & Clyde.
